Introduction
To mark World Suicide Prevention Day on 10 September, Faye Blackwell from the National Counselling Society (NCS) shares her thoughts on suicide prevention and what can be done to improve outcomes. Faye is Head of Engagement and Development at the NCS and has been a counsellor for over 20 years. She has personal and professional experience of suicide prevention and bereavement by suicide.
The NCS is one of the Authority’s Accredited Registers. We accredit a range of registers for therapies including counselling, psychotherapy and play therapy. We always recommend using a healthcare practitioner on a register we have accredited.
What Could Suicide Prevention Really Look Like?
According to suicide prevention charity Papyrus, suicide is the biggest killer of young people under 35 in the UK. On average, over five young people take their lives each day.
World Health Organisation statistics from 2019 suggest that the UK has the ninth highest suicide rate in the world.
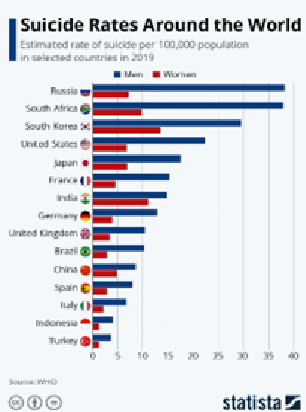
• Chart: Suicide Rates Around the World | Statista
While a better understanding of risk factors that contribute to suicide exists, improvements are still needed. What is missing from current suicide prevention strategy in the UK?
The solution may lie somewhere unexpected. By viewing suicide through a different lens, creating and embedding a shift in perspective and action across society, we could save more lives.
The power of shame
Normalising the dialogue around suicide helps to remove associated shame. Positive action has already been taken to modify the way we talk about suicide and move on from historic stigma. This needs to continue and filter into all areas of society, at a familial level, across education, health and mental health sectors and up to Government itself.
Professionals across the board need to model confidence and fearlessness when discussing suicide. And understanding the power of shame, the part it plays in suicidal feelings, and how our society feeds into that, is vital for suicide prevention.
Poverty and inequality
In its report The Mental Health of Children and Young People, The Children’s Alliance outlines how socio-economic factors contribute to increased poor mental health. The report describes how children from the most deprived households are four times more likely to develop serious mental health problems by the age of 11 than their more affluent peers.
The Samaritans’ report, Dying from Inequality, similarly recognises that 'People living in the most disadvantaged communities face the highest risk of dying by suicide…..financial instability and poverty can increase suicide risk. Suicide is a major inequality issue. Tackling inequality should be central to suicide prevention and support should be targeted to the poorest groups who are likely to need it most.'
Early intervention, better prevention
Research shows that with appropriate early intervention and support, suicide by young people can be prevented. In addition to amplifying the national voice as described above, we can help our children and young people (CYP) further, by providing safe spaces, both online and offline, where they can talk about their feelings freely.
Communication
Let’s go further and create a societal understanding of how children communicate, to improve our ability to support them. Verbal communication is not always easy for them, so they express feelings through behaviour. When this is punished or shut down, that child’s distress is unheard. We need to understand and explore a child’s behaviour, rather than treating it as ‘naughtiness’, and encourage and normalise the verbalising and expression of emotional narratives.
CYP are encouraged to disclose, yet worryingly, educational establishments are becoming risk averse and, in some circumstances, prefer to decline students a place, or remove them from their studies, because of declared mental health issues. This sends a detrimental message about the consequences of disclosing. If we ask children to speak up, we need to ensure a safe environment and system for them to do so.
Education
Valuing a child’s wellbeing over academic achievement is another key to suicide prevention, but is unlikely to be actualised soon. Recognising that educators are not trained mental health workers is achievable and important, for both the sake of pupils and teachers alike. Understanding mental distress in children requires specific training. Recommendations that all schools, colleges and universities have trained counsellors available need to be heard and acted upon. Counsellors in every educational establishment should be a statutory requirement, and a whole school approach (from early-years) to mental health be adopted.
Kate Day, Child Ambassador for the National Counselling Society and co-author of the Children’s Alliance report on children’s mental health, says, 'We must act now to prevent further deaths of our children and young people. Early detection of our child and adolescent suffering with their mental health is crucial to prevent further suicides. The continuing long waiting lists in child mental health services is putting our children at further risk.'
Prevention
Additional changes are achievable, include challenging the widespread belief that GDPR is more important than safeguarding, i.e. sharing information with family where appropriate.
All schools, colleges, universities and workplaces need to have clear pathways to, and availability of, crisis support.
Could we risk-assess public spaces through the lens of someone wanting to harm themselves - adding in compassionate signage and physical barriers where possible? How about training those who work in public areas? Could they ask someone, ‘Are you ok?’ or, ‘Can I help?’ rather than, ‘What are you doing here?’
Support and signposting
Despite encouragement for those at risk of suicide to disclose, what happens then? Overstretched services make referrals difficult or create delays in accessing help. A reliance on short-term, ‘quick fixes’, is a false economy. Long-term investment could produce longer-term benefits. There could be a case for shifting the emphasis from short-term ‘band-aid’ mental health approaches (Process-Centred), to implementing and valuing longer-term mental health strategies (Autonomy-Centred).
Support should not be time-restricted but provided according to need and for as long as necessary. Each suicide affects multiple people who are then at increased risk themselves. We need to engage with the peers of people who have died or made a serious attempt on their lives and provide trauma support.
The solution to saving lives lies in a societal shift
Perhaps the key to saving lives is in the fabric of our society, with a discourse of compassion and understanding, asking and listening, and practical measures, woven into every thread.
- Reduce shame around suicide – turn up the volume on the conversation.
- Start the conversation from early years. Give children a voice and the space to hear it.
- Better funding for state provision and/or the third sector is essential.
- Available and appropriate support for all, recognise (age/gender/cultural barriers to asking for help.
- Emergency intervention meetings when there is an emerging risk with a particular group.
- Understand that ongoing support (as opposed to a prescribed amount) may be required and should be needs-based.
- Training and advice for employers and employees - mental health and welfare being part of health and safety policies as standard - possibly as part of The Health and Safety at Work Act.
- Better communication between all groups/agencies involved.
- Reduce poverty, invest in hard-to-reach groups.
Find out more about how to check and find an practitioner on an Accredited Register using
check-a-practitioner
Find out more about World Suicide Prevention Day at Samaritans UK